I’ve talked about vaginal health before because it’s an important but often overlooked topic in women’s health. Breast health is another area we simply can’t afford to ignore. Sadly, breast cancer continues to be a leading cause of death in women and breast cancer rates keep rising. Mammograms are the go-to diagnostic tool for detecting breast cancer currently, but is a technology called thermography a better choice? I wanted to find out.
What Is Thermography?
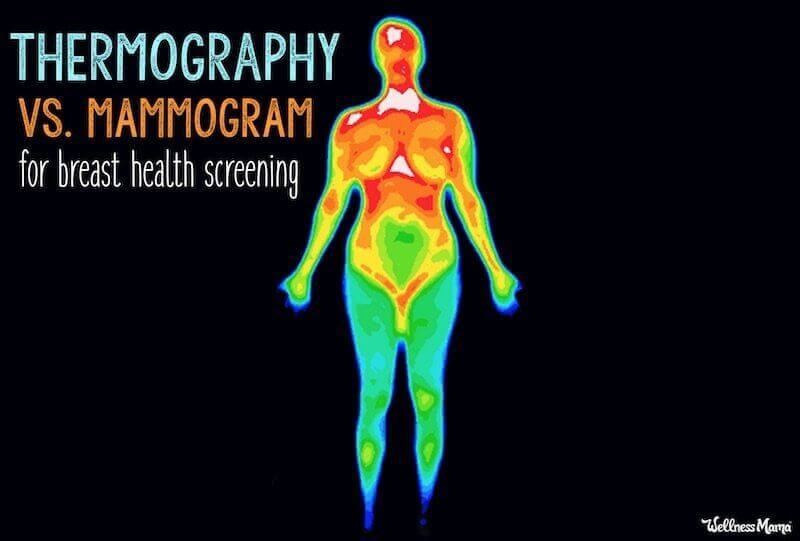
Thermography uses thermal imaging to detect existing or potential tumors. These images detect small variances in temperature, which may be a sign of tumors (or even places where a tumor may grow in the future). This is because there is more blood flow at the site of cancer cells, so a warmer part of the image may indicate cancer.
Typically a baseline image is created (around age 25 if possible) and future images are compared to the baseline image. Each person’s image is unique but should stay the same over time. If it doesn’t, it may be a sign of disease.
In this post, we will focus on the benefits and risks of thermal imaging or thermography as compared to mammograms.
The Case for (or Against) Routine Mammograms
Mammography has been the go-to diagnostic tool for breast cancer since the 1970s. Since then guidelines have changed and the U.S. Preventive Services Task Force now recommends mammograms only for women aged 50-74 every two years. They recommend screening on an individualized basis for women 40-49, “weighing the benefits and harms of screening every two years.” Younger women are not recommended to get mammograms.
Unfortunately, many women aren’t given the risks of mammograms and are under the impression that mammograms always save lives (which they certainly do in many cases). These new guidelines came about in response to new research that shows mammograms may be ineffective for certain groups (like younger women).
While this is a good start, women may not be told the following about mammograms:
- They may not reduce deaths – A Cochrane review of randomized controlled trials of nearly 600,000 women found that though mammograms increased early diagnosis of breast cancer, they did not reduce the number of women who died from breast cancer. The review states: “For every 2000 women invited for screening throughout 10 years, one will avoid dying of breast cancer and 10 healthy women, who would not have been diagnosed if there had not been screening, will be treated unnecessarily.”
- There are potential risks from radiation – Mammograms expose us to radiation. The amount of radiation isn’t a huge amount (less than many other x-rays) but could add up over time.
- Radiation risk varies by individual – Women with a genetic mutation (germline mutations in a DNA-damage control pathway) may be at higher risk for radiation-induced cancer and should carefully consider whether a mammogram is worth the risk.
- False positives are possible – As with almost any diagnostic tool, there are going to be false positives. One study found that there was an overdiagnosis rate of 24.4%. It also found that in younger women (below the screening age) the overdiagnosis rate rose to 48.3%.
- False negatives are also possible – False negatives are another concern. About 1 in 5 women will get a false negative. False negatives are more likely to occur in breasts that are dense (younger women have dense breast tissue, which is one reason routine mammograms for younger women are not recommended). Mammograms aren’t a 100% accurate diagnostic tool but women with a clean mammogram may ignore symptoms thinking there’s no way they have cancer.
Researchers in this 2014 JAMA review on the benefits and risks of mammograms highlight the intensely personal and individualized nature of breast cancer screening decisions:
Each woman may feel differently about the possibility of having a false-positive result or being diagnosed with and treated for cancer that might not have caused problems. It is important for you to consider what these experiences might mean for you. It is also important to consider how you might feel if you decide not to undergo screening mammography and you are later diagnosed with breast cancer, even if the likelihood that mammography would have made a difference is small.
As always, a personal discussion with your doctor is the best place to start.
Benefits of Routine Thermography
Here are some reasons to consider thermography vs mammogram for breast imaging.
Note: Thermography must be done by a knowledgeable technician in a facility that is backed by qualified, board-certified physicians. A technician that doesn’t know how to read the imaging won’t be helpful.
- Less invasive – Thermography doesn’t require any compression, which is more comfortable for the patient.
- May detect “pre-cancer” areas – Since thermography uses heat to look for disease, it can potentially find a place in the tissue that would turn into cancer (but isn’t cancer at the time of screening). This information could be very helpful in preventing cancer. The treatment would then be focused on diet and lifestyle changes that could help reverse the disease.
- Good for young, dense breasts – Since mammograms aren’t very useful for young women, thermography could be a better tool for young women at risk (a close member of their family had breast cancer, for example).
- Detects cells in armpit area – Thermography also can detect cancer cells in the armpit area which mammograms are notoriously bad at catching. In fact, thermography can be used for the whole body (though research focuses on breast cancer detection).
- Safety – Thermography is safe and can be used during pregnancy and nursing.
Thermography is most accurate when baseline images are started early (around age 25).
Drawbacks of Routine Thermography
While thermography may be a helpful tool, it does have some drawbacks too.
- Expense – Most insurance companies won’t cover thermography since it’s not part of the standard of care. It can also be difficult to find a thermography center in some areas (most hospitals don’t use them).
- Sensitivity and specificity questions – A small study found that thermography had a 97 percent sensitivity rate (it caught 97 percent of cancers) but only a specificity rate of 44 percent (meaning it over diagnosed 66 percent of women without cancer). The researchers thought that the bad specificity rate could have been because the study was on women who already had suspicious mammograms or ultrasounds.
Thermography as a Piece of the Whole
Thermography is an alternative (or addition) to mammograms that may work for some women. While thermography seems to have promise as a diagnostic tool, it’s not recommended as an alternative to mammograms especially when diagnosing a tumor that was found in a manual exam.
However, thermography done in conjunction with other diagnostic tests will give the best picture. Your doctor may use thermography and ultrasound first, for example, and then a mammogram if something looks suspicious. Talk with your practitioner to see what options are available.
Thermography vs. Mammogram: Final Thoughts
When it comes to breast cancer, early detection is great, but prevention is even better! Whether mammograms, thermography, or some other technology is best, it’s still only a tool and can’t give 100% accurate information. It’s great to do our homework and be aware of the benefits and risk of the technologies available, but we must continue at the same time to make breast health a priority through regular healthcare, frequent breast self-examination, and a healthy diet and lifestyle.
This article was medically reviewed by Dr. Shani Muhammad, MD, board certified in family medicine and has been practicing for over ten years. As always, this is not personal medical advice and we recommend that you talk with your doctor or work with a doctor at SteadyMD.
Have you used thermography? What was your experience?



Leave a Reply