Root canals are a controversial topic in the dental world (if you didn’t know!). I’ve always had a fascination with studying oral health, and while I’m glad to have never needed a root canal (or an alternative), I felt it was good to research them and be prepared in case I ever did.
Many dentists consider the root canal—a dental procedure to treat deep dental cavities—to be a safe procedure, while other research has shown that root canals may allow dangerous bacteria to grow in the mouth and the rest of the body.
What Is a Root Canal?
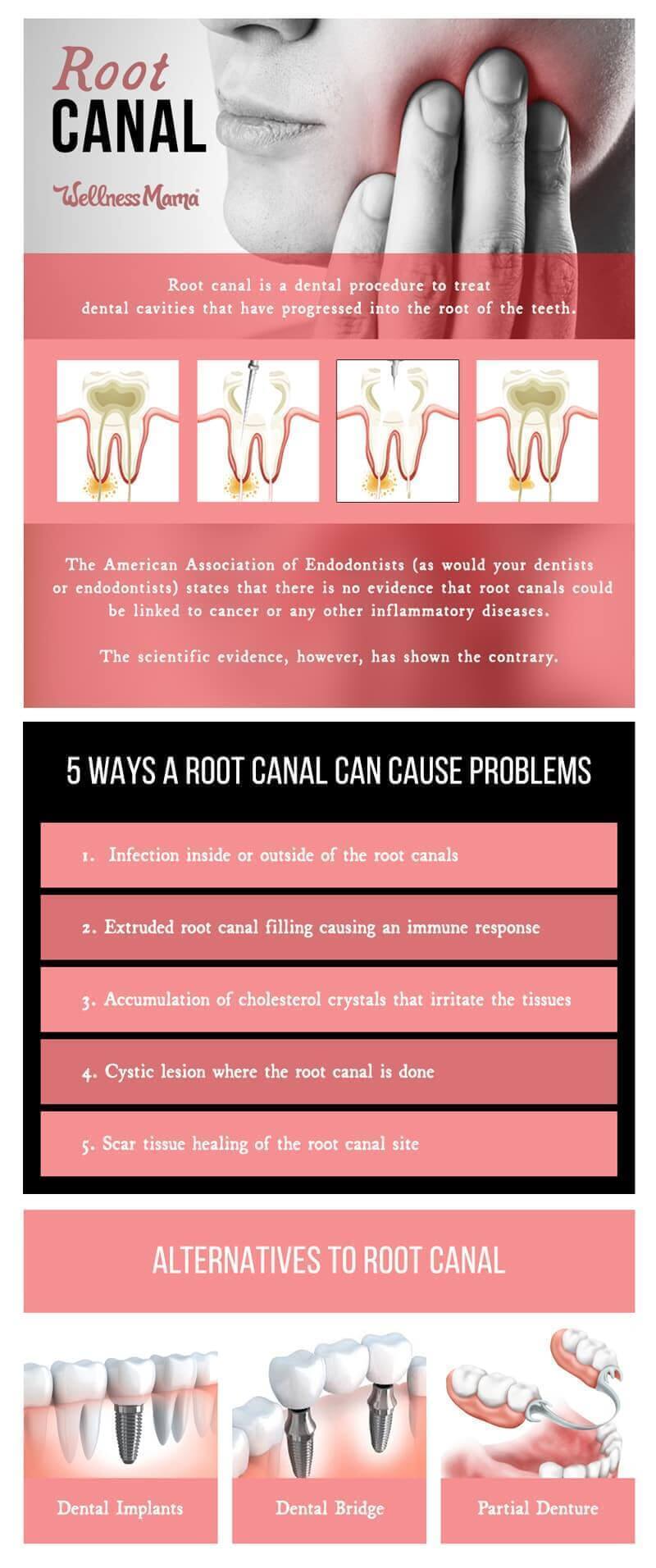
Root canals are recommended for dental cavities that have progressed into the root of the teeth. The treatment of such cavities requires that all the infected pulp inside of the teeth be removed and cleaned, before the dental filling materials are injected into the tooth.
This allows the patient to keep the tooth, although the living tissue inside of the tooth is replaced, and the tooth is considered dead.
Is a Root Canal Safe?
This is where things start to get confusing, and it really depends on who you ask.
On the one hand, the American Association of Endodontists states that there is no evidence that root canals could be linked to cancer or any other inflammatory diseases. On the other hand, some scientific evidence shows there could be a potential for some pretty serious problems.
So Who Is Right?
Let’s look at the data.
One study tested the effectiveness of root canal cleaning procedures and found endotoxins and pathogenic bacteria in 100% of root canals. The cleaning procedures can clear up to 44% of these bacteria, but the bacteria always persist.
The theory is that this could lead to long term problems, including some pretty serious ones. In fact, there are five ways that a root canal can lead to problems, including:
- Infection inside or outside of the root canals
- Extruded root canal filling causing an immune response
- Accumulation of cholesterol crystals that irritate the tissues
- Cystic lesion where the root canal is done
- Scar tissue healing of the root canal site
Even after the root canal procedure is long over, it appears that bacteria can (and often does) remain. This can logically lead to infections and other problems, and antibiotics are often given if needed.
However, while antibiotic use presents its own side effects, one study has shown that antibiotic use does not significantly reduce pain and swelling. Overall, there is no strong evidence suggesting that antibiotics really help with root canal infections.
The Problem with Lingering Bacteria
The bacteria (again, present in 100% of all root canals) can stimulate inflammatory molecules such as Interleukin-1beta and TNF-alpha, thereby raising inflammation throughout the body.
In severe cases, this can cause fever, malaise, and abscess or cellulitis in the head and neck area that may even require hospitalization.
Even without major complications, the bacterial toxins and inflammation can lead to seemingly unrelated health problems, as Dr. Weston A. Price discovered.
Weston A. Price on Root Canals
Dr. Price, a dentist known for his work on the relationship between nutrition and dental health (and overall health), was able to show that root canals can cause chronic diseases of inflammation by experimenting on rabbits.
Here’s what he did:
He conducted a series of experiments on rabbits, using extracted teeth from people with various health problems. His research found that rabbits would develop the condition that the person with the tooth had.
In other words: when using a tooth from a person with heart attacks and arthritis, the rabbit implanted with the root canal tooth would develop heart attacks and arthritis within a few weeks.
Back to the Bacteria
The bacteria that are found inside of root canals include groups of bacteria called Fusobacterium, Parvimonas, Prevotella, Porphyromonas, Dialister, Streptococcus, and Treponema.
Many of these bacteria are naturally present in the mouth, but they only become a problem when we are infected with them. When they grow in the root canal, the anaerobic conditions inside the root canal can cause these bacteria to become more dangerous. In addition, the ecosystem of these bacteria can make them even more dangerous.
These bacteria, in the context of periodontal infections, are linked to many chronic inflammatory diseases:
- The bacteria Fusobacterium, Porphyromonas, and Treponema are linked to atherosclerosis.
- The bacteria Porphyromonas is linked to Alzheimer’s disease through its ability to create inflammation in the body.
- Porphyromonas, Treponema, and Tannerella are linked to poor blood sugar control and diabetes.
Because these bacteria are transmissible, it explains why the exact same diseases could be transmitted from humans to rabbits by tooth transplantation in Dr. Price’s experiments.
This list of links between root canal bacteria and diseases is by no means exhaustive, but the literature has consistently shown that the infections of these bacteria in the mouth are linked to chronic inflammatory diseases.
Root Canals: What to Do?
After researching, I would personally choose not to get a root canal if I was ever told I needed one. There are some less well known alternatives, but they also all present their own challenges. The best option, of course, is to maintain optimal oral health as much as possible and hopefully never have to make this decision.
Pros and Cons of Getting a Root Canal
Unfortunately, when a tooth has progressed to the point of needing a root canal, there aren’t any really great options. And even within the dental community, the recommendations vary widely. As this article explains:
Dentists who speak out against the safety of root canals bring up 3 main concerns:
- There is no way to completely remove all the dead tissue from the tooth
- There is no way to sterilize the tooth, thus leaving bacteria in the tooth
- The materials used to fill the hollowed out tooth leak and cause problems “downstream”
Those in the profession who claim that root canals are safe claim:
- Enough of the tissue is removed
- The body’s immune system can better get on top of any existing infection
- There are improved substances to fill the tooth
- There are no other suitable options
Alternatives to Root Canal Treatment
As explained above, the bacteria present in dental cavities can be quite dangerous. Deep dental cavities should certainly be taken care of, especially those that have the potential to infect deeper in the jaw.
So if a root canal isn’t the best option, what is?
Some holistic dentists suggest that if the dental cavities are deep, the tooth should be extracted with the periodontal ligament removed to prevent further infections. Of course, this leaves a person without a tooth, though there are now several options if a tooth has been removed, such as:
Dental Implants
The tooth with cavity is removed and replaced with a metal implant. It still remains controversial whether the implantation of metal to replace the tooth can cause problems as this can raise the levels of such metals in the body and cause an immune response.
Dental Bridge
This may be a safer option than dental implants since the metal is not implanted into the gums in the same way.
Partial Denture
A removable denture to replace the extracted tooth is the least invasive option.
What to Do with Existing Root Canals
There is enough information (and enough conflicting opinions) when it comes to root canals to make a person’s head spin! Hopefully, the emerging research will shed some light on the safety of root canals in the future, but what about people who already have one or more?
Get a Second Opinion
A modern-day researcher, Dr. Boyd Haley at the University of Kentucky, completed follow-up research to Dr. Price’s work and his findings are telling:
Roughly 25% of the root canal teeth studied had bacteria within them which produced toxins that were fairly benign. 50% of the teeth studied contained bacteria within their structure that would challenge a healthy immune system. The last 25% of the teeth contained bacteria which produce toxins more powerful than botulinum (Important note, botulinum is widely recognized as the most toxic substance known to humans). This bears repeating. 25% of the teeth Dr. Haley studied contained a toxin stronger than the strongest toxin known to humans…
Many holistic health experts, including Dr. Mercola and many of his dentist colleagues, recommend removing the infected teeth and root canals, even if they look and feel fine. Dr. Haley, who did the above study, had his teeth with root canals removed after completing his study.
Because every dental procedure comes with a risk (not to mention the expense), it is best to consult a biological dentist who is well versed in Dr. Price’s work. I would suggest the same when considering wisdom tooth removal or any other surgical dental procedure.
Adjust Lifestyle Choices
Thanks to modern lifestyles, we all know that the incidences of heart disease, Alzheimer’s, and diabetes are on the rise. Based on the research of Dr. Price and Dr. Haley, it appears that root canals may contribute to a subset of the cases.
Personally, I’d choose to have a tooth pulled instead of getting a root canal if I ever had to make the choice. I’d rather lose a tooth than have a risk of long-term inflammation and other conditions (of course, once you’ve gotten a cavity, starting on a remineralization routine is a good way to keep from needing a root canal in the future).
Some sources suggest that if it isn’t possible to avoid or remove a root canal, certain lifestyle factors may help mitigate any potential problem. In fact, these are things we should probably be doing anyway, including:
- eating a low inflammatory diet
- managing stress
- maintaining gut health
- using plant extracts like aloe vera, rosemary, or eucalyptus that have some antimicrobial extracts against bacteria that infect the teeth and root canals. (However, there is no clinical study demonstrating the safety and effectiveness of these substances in real human root canals, as we still don’t know how well these substances … or even antibiotics … can reach the blood that flows in that area.)
- Choose safe and effective dental products (like Wellnesse toothpaste!) to maintain good oral health
Root Canals: Bottom Line
Root canals are a tough subject. There certainly isn’t a clear and completely safe solution. I think all dentists would agree that the best scenario is to have great oral health and avoid ever needing this controversial procedure if at all possible.
For those who already have or need a root canal, it may be helpful to find a trusted dentist to help explore the options.
Additional Reading & Resources
- 3 Questions to Ask Your Dentist about Root Canals
- I Have a Root Canal, What Are My Options?
- Understanding the Issues with Root Canals
This article was medically reviewed by Dr. Steven Lin, who is a Board accredited dentist trained at the University of Sydney. With a background in biomedical science, he is a passionate whole-health advocate, focusing on the link between nutrition and dental health. As always, this is not personal medical advice and we recommend that you talk with your doctor or dentist.
What’s your take on root canals? Please weigh in in the comments below.




Leave a Reply